This paper discusses why radiation exposure in medical imaging is such a hot topic, how a dose management solution can help healthcare organizations to lower dose levels and the important features of such a solution.
An increase in radiation dose exposure
In 2006, the average annual effective dose per individual in the US was6.2 mSv1, a figure that has almost doubled over the last 25 years [1]. Approximately 50% of the dose currently received stems from background radiation [1], but varies depending on where you live (for example, in Australia dose levels are about half of levels in the US) [2]. The other 50% of the radiation we receive comes from medical imaging, that is man-made radiation, which is the underlying reason for the doubling in dose levels [1]. The trend for exposure from background and medical radiation to the US population is illustrated in Figure 1.
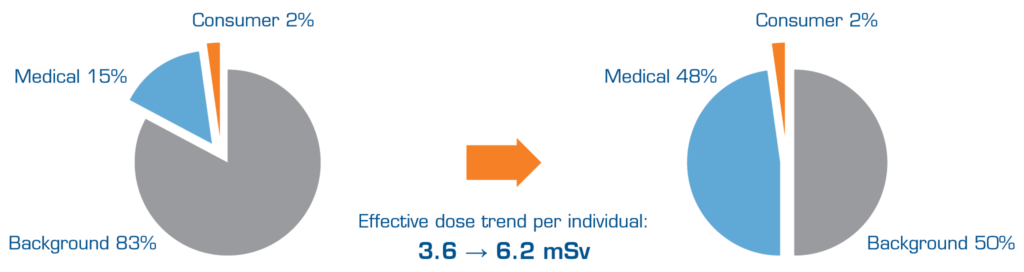
Figure 1. Radiation exposure trend for the U.S. population. (Remade charts from [1], occupational/industrial radiation exposure neglected in this image.)
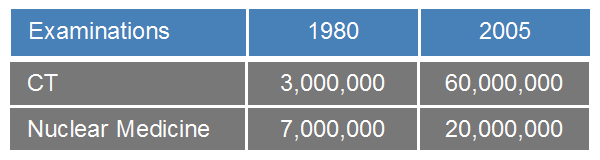
Figure 2. Growth of computed tomography (CT) and nuclear medicine examinations in the United States. (Remade table from [6], P. 273.)
Although the average dose of ~3 mSv from medical imaging is currently much higher than in 1980, one should bear in mind that the average does not say much for each individual. An average calculation takes into account people that have not been exposed to any medical radiation at all, as well as people that have conducted several examinations and been exposed to significantly higher radiation dose levels. However, averages are useful when studying the collective dose2 on the entire population and its total health effects, or when providing hospitals with dose levels for specific studies for benchmark purposes. Knowing that radiation has adverse health effects, the increase in the average radiation dose has created concerns both in healthcare and at political levels.
Uncertainty about the cancer risks causes concern
For a long time, it has been known that ionizing radiation in high doses increases the risk of developing cancer, but the danger posed by lower doses such as those from medical imaging is still controversial. Since radiation is a very weak carcinogen it is difficult to isolate radiation-induced cancers that are superimposed on the normal background risk for other cancers. Approximately 40% of the population will be diagnosed with cancer at some point in their life from causes unrelated to radiation. Estimating the risk of an exposed patient to developing cancer requires expressing the dependence of risk on radiation dose as well as gender and age on exposure [4].
There have been some studies trying to quantify the increased cancer risk due to low radiation doses, many of these were conducted on the survivors of the atomic bombs in Japan. One study predicted that 1 individual in every 1,000 would develop cancer from an exposure to 10 mSv [4]. Other research showed that radiation dose levels exceeding 50 mSv resulted in a statistically significant increase in the occurrence of cancer [5]. These research results are very approximate and should not be used to conclude the risk posed by one single CT scan. However, it is rather concerning that some CT and nuclear medicine examinations give estimated doses in the range 10-25 mSv, and some patients receive multiple examinations [6].
What can be concluded is that we do not know how dangerous the increase in radiation exposure is and that care should be taken to keep radiation dose levels as low as possible. The main task for healthcare will be to find a balance between the benefits of imaging exams and the risks posed by conducting them [7].
Lowering doses requires a holistic approach
The significant increase in radiation exposure and uncertainty regarding the risk of cancer have raised concerns leading to a recent change of direction within medical imaging. Several initiatives to lower dose levels are being established and many healthcare providers have initiated dose reduction programs to guard patient safety and to comply with new regulations.
To significantly lower the radiation exposure to patients, a holistic approach is necessary throughout the healthcare organization and procedures for lowering dose levels need to be implemented as part of each hospital staff’s routines. The change of peoples’ habits is hard and should be implemented incrementally and iteratively without sacrificing diagnostic quality [8].
Information and integration are key to lowering radiation doses
There are two main kinds of information required to trigger such a change. First, is knowledge of why it is important and how to lower doses. This information needs to permeate down to all parties involved including referring physicians, radiologists, radiographers, medical physicists, hospital management, IT staff and patients. The aim is to create an understanding that dose levels should be included in decision making and that people have to change their way of working.
Secondly, examination data needs to be collected, including data about dose levels, equipment, performing physicians, referring physicians, etc. This will not only allow for comparisons of dose levels, but it will also allow investigations of the underlying reasons for high radiation exposures.
A dose management solution is an effective tool for automatically collecting, monitoring and providing easy access to dose information, which is necessary for follow-up of a hospital’s progress in reducing dose levels. Comparing average dose levels is fundamental when identifying the magnitude of reductions needed in radiation dose levels and to provide a benchmark against which the effectiveness of reduction efforts can be measured [8]. A dose management solution should continuously communicate the performance data on dose reduction from as many stages of the Imaging Cycle (see Figure 3) as possible, which will then act as a basis for further training of staff.
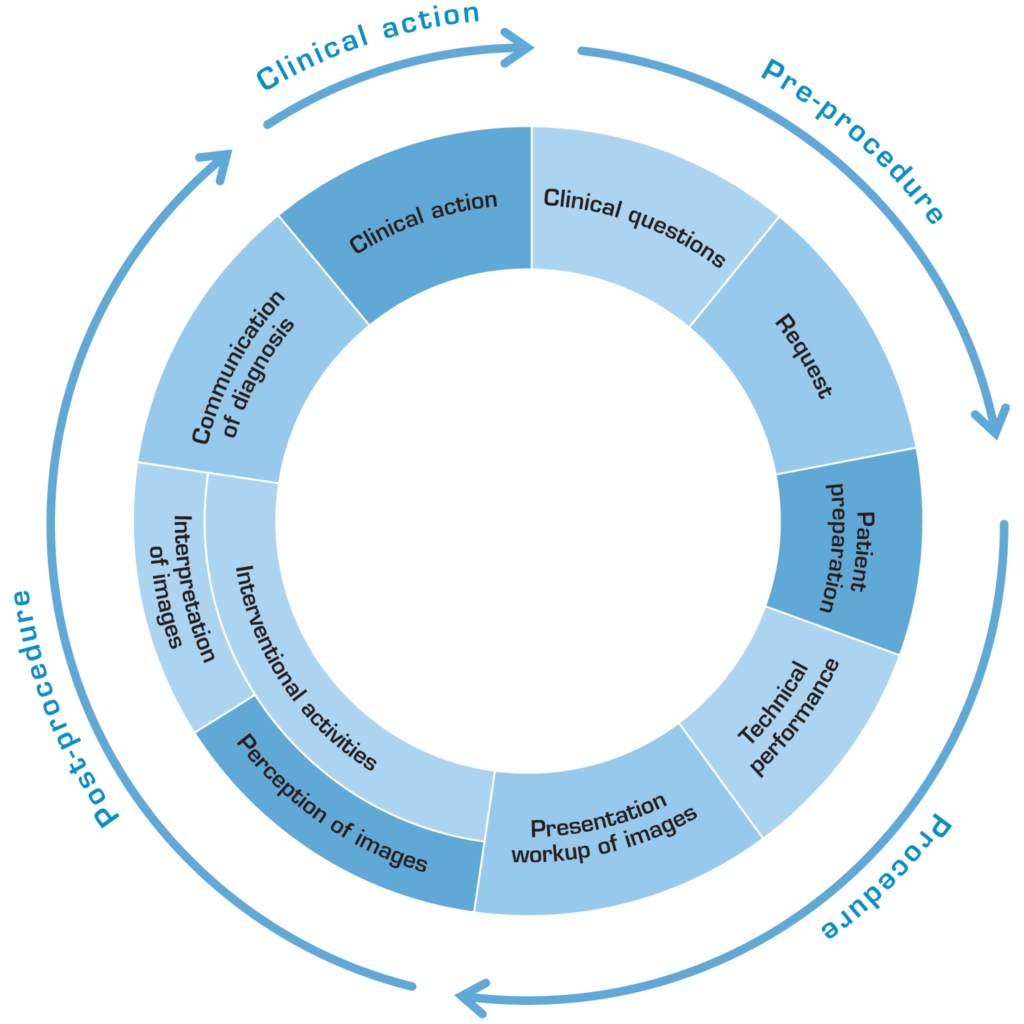
Figure 3. Stages of the Imaging Cycle that all should be aware of for lowering patient doses. (Remade picture from [9].)
Integrating the dose management solution with other vital hospital IT systems will make the reduction of dose levels part of the workflow and the hospital’s existing routines. Integration is key to prevent the dose management solution from becoming “just another IT system to log in to,”
The selection of dose management solution
The medical imaging industry is under change and many medical providers are today using, or are considering starting to use, some kind of dose management solution for the collection and monitoring of dose levels. The system should be the spine of the dose reduction program providing dose information to all stages of the Imaging Cycle to create awareness and measure performance.
Selecting a sophisticated dose monitoring solution will not only provide the hospital with a tool for lowering doses, but will provide a system to ensure the quality of care. To leverage the value of the solution, healthcare providers should make sure that it integrates with other vital hospital IT systems and becomes a part of the daily routines.
The selection of a dose monitoring solution can be a complex decision to make for a healthcare provider. Based on the discussion in this paper, some of the most important features to look for have been stated below:
Integration
- Ability to integrate several different hospital IT systems (e.g. via HL7 connections) to be able to provide information to all roles involved in the Imaging Cycle.
- Ability to update on changes in other IT systems to create a uniform dataset across the hospital (e.g. changed names on patients).
- Automatic collection of dose information from all modality types and the ability to report dose levels to authorities.
Information
- Allow for comparison of dose levels between different equipment to guide new purchase decisions, maintenance and utilization of low-dose equipment.
- Allow for comparisons between radiation dose levels given by specific staff and departments for identification of training needs.
- Identification of over-radiation cases by sending system alerts when a threshold has been exceeded, and allow for easy drill down to find all the information related to the examination needed for further investigation.
- Easy access to the entire patient dose record to avoid unnecessary examinations and provide an opportunity to select other kinds of examination types.
- Allow for optimization of protocols by comparison of examination dose levels.
References
[1] National Council on Radiation Protection and Measurement, “Ionizing Radiation Exposure of the Population of the United States: NCRP REPORT No. 160,” Radiation Protection Dosimetry, vol. 136, no. 2, 2009.
[2] WNA, “Nuclear Radiation and Health Effects,” World Nuclear Association, 2013.
[3] M. R. Tracy L. Herrmann, E. R. Terri L. Fauber, P. R. Julie Gill, R. Colleen Hoffman, M. R. Denise K. Orth, M. R. Paulette A. Peterson, B. R. Randy R. Prouty, M. R. Andrew P. Woodward and B. E. Teresa G. Odle, “Best Practices in Digital Radiography,” American Society of Radiologic Technologists, 2012.
[4] National Research Council, “Health risks from exposure to low levels of ionizing radiation. BEIR VII Phase 2,” National Academies Press, Washington, DC:, 2006.
[5] D. Pierce and D. Preston, “Radiation-induced cancer risks at low doses among atomic bomb survivors,” Radiation research, no. 154, pp. 178-186, 2000.
[6] S. E. Amis, P. F. Butler, K. E. Appelgat, S. B. Birnbaum, L. F. Brateman, J. M. Hevezi, F. A. Mettler, R. L. Morin, M. J. Pentecost, G. G. Smith, K. J. Strauss and R. K. Zeman, “American College of Radiology White Paper on Radiation Dose in Medicine,” American Collage of Radiology, 2007.
[7] Food and Drug Administration, “Initiative to Reduce Unnecessary Radiation Exposure from Medical Imaging,” Center for Devices and Radiological Health, U.S. Food and Drug Administration, 2010.
[8] E. Tamm, J. Rong, D. Cody, R. Ernst, N. Fitzgerald and V. Kundra, “Quality initiatives: CT radiation dose reduction: how to implement change without sacrificing diagnostic quality.,” RadioGraphics, pp. 1823-1832, 2011.
[9] A. Wallace, “Presentation: ARPANSA Web Based National Diagnostic Reference Level Survey Solution,” Australian Radiation Protection and Nuclear Safety Agency, Melbourne, 2013.
Footnotes
1Sievert (Sv) is the SI derived unit of effective dose. Quantities measured in Sieverts are designed to represent the stochastic biological effects of ionizing radiation.
2Collective dose is the sum of all the effective doses received by an exposed population and can be used to estimate the total health effects of a process or accidental release involving ionizing radiation.
3EHR – Electronic Health Records, is digital documentation of an individual’s medical history.
4PACS – Picture Archiving Communication System, a IT system providing storage and distribution of digital images.
