Region Skåne has one of the largest digital pathology implementations in the world. The region produces over 800,000 histopathology glass slides per year, and the digitization came as a result of the need to shorten cancer care lead times in the region. In total, there are 14 scanners—and more to come—connected to one centralized enterprise management system for all medical images. The system is utilized across four labs located in the cities of Malmö, Helsingborg, Lund and Kristianstad. In the midst of the coronavirus pandemic, we met with Kevin Sandeman to talk about the implementation, the challenges and some of the key factors that prompted the move to go fully digital in such short time.
We have now reached a state of peace of mind and I do not think many pathologists want to go back to their microscopes. The digital workflow saves a lot of time and reduces the risk of errors, missing glass, and mix-ups.
When did you finish the pathology digitization in Region Skåne?

Kevin Sandeman, Department Manager at Region Skåne’s pathology lab in Malmö
Kevin: The project ran during 2019 with scanning starting in May. Since November 2019, we have been completely digital with regard to all histopathology. Today, in April 2020, we have also taken steps to start digitizing our cytology. So far, we only scan cytology cases for conferences.
We have now also started to scan immune-fluorescence cases for clinical use in the city of Malmö. This has been made possible by having access to some of the latest technology—both in terms of the software to be able to diagnose such images, and the scanner hardware to acquire the images. I am very pleased to have access to Region Skåne’s enterprise imaging platform. It is used for all medical imaging in the Region and has enabled us to digitize in full scale in a very short period of time.
What kind of software and scanners do you use in Region Skåne?
The software is a centralized enterprise image management system from Sectra. It handles all the region’s medical images including radiology, dermatology and other multimedia. This allows various specialists to gain access to each other’s images and reports, which has been proven to facilitate the work significantly. The system is then integrated with our LIMS—both on the server side to receive necessary case information, but also on the desktop level to ensure the right images are displayed for the right case. The LIMS integration is key to achieving a good workflow.
In the region, we have a total of 14 scanners. At each of the four labs, we have at least one normal scanner and one scanner for macro slides. Furthermore, the grossing images are imported to the enterprise imaging system.
Has the scanning time been a problem?
The lead times in the region were about two to three weeks before we started scanning, so the scanning time of four hours has not been something that has caused any issues. High-priority cases are handled without delays. We run batches all days, as well as one batch overnight.
One important key takeaway is that we scan everything in 40x magnification. This reduces the need for re-scanning. Together with the work we conducted in the lab, we have succeeded in reaching a re-scanning level of less than 1 percent, which is considered extremely low.
The close collaboration we have enjoyed with Sectra has been key to the acceptance among pathologists. It motivates them to adopt the new technology.
What have the pathologists’ responses been to the digitization?
In the beginning, many were skeptical. A lot of questions were raised regarding quality. We solved this initially by handing out the slides and providing access to the digital images in parallel for double reading. All difficult or ambiguous cases were gathered in a specific file and discussed later in a group with pathologists, managers, and lab technicians. In this group, we discussed both the cause and the solution to the potential lack of quality or discrepancies found. In almost all cases, we could conclude that the digital format was not the cause of the issue. Most issues resulted in adjusting the tissue preparation phase to optimize the scanning.
We have now reached a state of peace of mind and I do not think many pathologists want to go back to their microscopes. Now they only have access to the digital images, and all manual workflow steps, such as managing paper pieces and wooden glass trays, have been eliminated. The digital workflow, including digital annotations and instant image access, saves a lot of time and reduces the risk of errors, missing glass, and mix-ups.
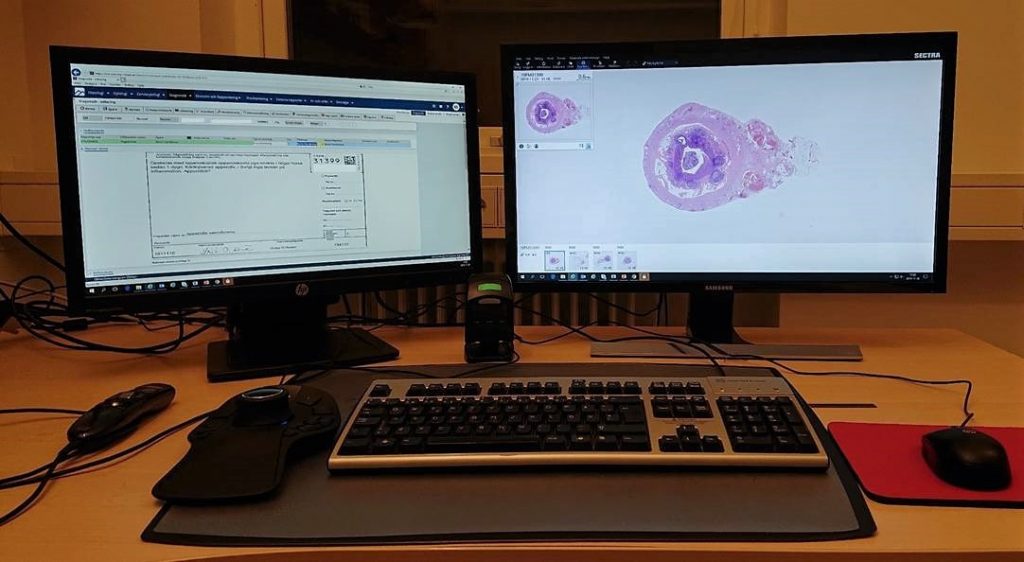
<em>One of the digital pathology workstations in Region Skåne.</em>
You mentioned quality issues; how has the quality been affected?
Initially, we had to make numerous changes to the tissue and glass preparation steps to enable the scanners to produce good-quality images. For example, we now section every glass at four micrometers instead of six. In the end, we have succeeded in reaching a very low reject rate from the pathologists. Only 10 out of 1,300 images are sent for re-scanning due to unsatisfactory sharpness.
All in all, I can say that the lab has worked very hard to ensure high-quality images are produced. It turned out very well in the end. Largely thanks to our fantastic staff.
What is your main advice to eliminate the hurdles?
A key has been to resolve issues continuously. Pathologists do not have the patience or time to wait, so we had to resolve issues extremely quickly as they occurred. For example, lab technicians have been trained to assess image quality before the digital images are made available to the pathologists.
One success factor has been the close collaboration with Sectra. We have worked together with their product team to specify requirements, which have been implemented within a couple of months. The short time between concept and action has led to pathologists to feel part of the process and this has considerably facilitated the adoption.
Before, we had two full-time lab technicians that handled the assembly and sorting of cases to pathologists. Today, one lab technician spends about three hours on this task and they do other activities instead.
Has the digitization improved productivity?
Well, the scanning of slides involves an additional step, but we have been able to justify the additional time it takes by more efficiently utilizing our resources. For example, we save a lot of time by not having to send physical slides around anymore. Once the images are digital, they can be reached from anywhere, anytime.
So far, the big win has been made in the lab. After the slides have been scanned, the lab technicians do not have to look for glass, transport them, or read their IDs anymore. Everything is much more streamlined, and we have been able to remove many manual and time-consuming steps for the lab personnel. One concrete example is that before, we had two full-time lab technicians that handled the assembly and sorting of cases to pathologists. Today, one lab technician spends about three hours on this task and they do other activities instead.
Another example is that the preparations for our multidisciplinary rounds have gone from two days of work for some, down to two hours. That is just remarkable.
We are conducting measurements to quantify the overall productivity increase, but it is still too early to say.
What are the major advantages you have experienced so far by going digital?
We actually made a list of the biggest advantages we have seen:
- Ergonomics
- Slides are always available—anywhere and anytime
- More efficient consultations, diagnostic support and workload balancing between units
- Facilitating multidisciplinary rounds on local, regional and national level
- More efficient training: Having full access to the archive, annotation and discussion has resulted in residents learning a lot faster
- Enhanced management capabilities: We have an overview of outliers, lead times and the ability to monitor and react
- Integrated diagnostics: Since we use the same system as our radiology department, we have access to each other’s reports and images. This has considerably improved diagnostics
- For example, MRI prostate where the radiologists need quick feedback on what they have seen, and accessing pathology images and reports has improved this workflow
- Also, the pathologists benefit from seeing radiology images to locate where the biopsy has been taken. For example, the dermatologists have shown a great appreciation of having access to pathology material
The digitization has given us a tool that enables us to both see lead times and to act on them.
You mentioned workload balancing between labs, can you tell us more about that?
Now that all slides are digital, we have a complete overview of the workload at each site as well as per organ type. We also see the current status of lead times and can immediately take a management decision to reallocate resources to support those labs experiencing a higher workload or suffering from absences due to sickness. This can be compared to the previous workflow, where it took three days to pack, send, and unpack glass when redistributing workloads between the labs.

<em>Quality review by a pathology lab technician in Region Skåne.</em>
What is the next step in the digitization journey?
The image viewer is already very intuitive and fast, but together with Sectra I think we can make some smaller optimization steps.
The second step we currently work with is the implementation of artificial intelligence (AI) based image analysis tools. We are closely monitoring how the market for such applications is developing. There is a wealth of narrow applications for specific purposes, so we see a need for a platform to gather these and integrate them into the software. The EU legislation of how AI should be used is still difficult to interpret and not yet harmonized.
We are currently in the midst of the global COVID-19 crisis. How has this impacted your pathology department?
At this moment (April 13, 2020), Region Skåne is in preparation mode. Elective surgeries have been partially postponed, and the volumes have declined sharply. This has resulted in significantly lower volumes for us at the pathology labs. We are not directly involved in the COVID-19 diagnostics, and at the moment we are prepared to react in case laboratory personal fall ill.
Even if the digital workflow in theory allows pathologists to work from home, we are not yet doing this to a great extent. It is valuable to have pathologists onsite to be able to have close dialogue with lab technicians, trainees, and colleagues. However, the digital workflow has given us the opportunity to work from home if so needed, and we also see great benefits with the easier workload balancing if pathologists were to fall ill.
Recorded video webinar with Q&A
Featured products & services
Related cases



